A deviated septum operation may help improve breathing when a crooked septum is causing ongoing congestion, sleep disruption, or frequent sinus problems. Septoplasty can be a good option for the right patient, but it’s important to weigh the benefits, risks, and expected septoplasty recovery before deciding whether surgery makes sense.
Why does a blocked nose affect more than breathing
Living with a blocked nose affects more than you might think. Some people deal with constant stuffiness on one side, trouble sleeping, mouth breathing, or recurring sinus pressure that never seems to fully go away. When medications and home care haven’t helped enough, it’s natural to wonder whether surgery could finally bring relief.
If you have a deviated septum, understanding the pros and cons of septoplasty, what to expect during recovery, and whether a deviated septum operation is truly necessary helps you make a more confident decision.
What septoplasty is and why it’s done
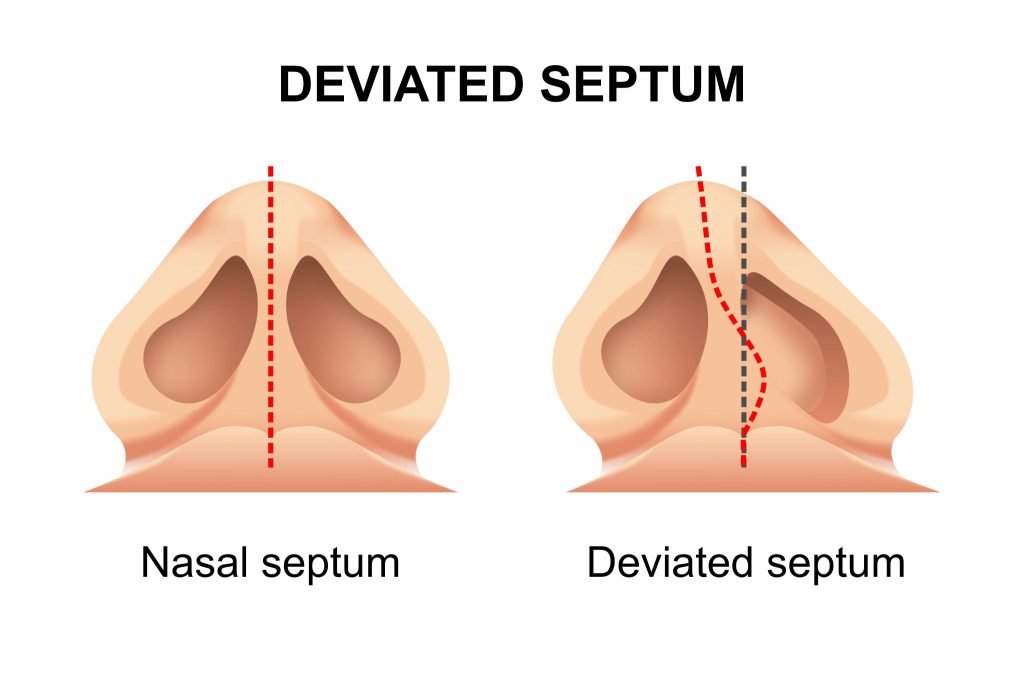
A deviated septum means the wall inside the nose is off-center enough to affect airflow. Many people have some degree of septal deviation, but symptoms usually occur when that shift blocks one or both nasal passages, making breathing harder.
Septoplasty is a procedure that straightens the septum to improve airflow. It’s a functional surgery, which means the goal is to help the nose work better. For the right patient, it reduces nasal blockage, improves comfort, and makes breathing easier throughout the day and at night.
Surgery isn’t always the first answer, though. Allergies, inflammation, enlarged turbinates, or a mix of issues may also cause nasal obstruction. That’s why the real question is whether the septum is truly the main reason for the breathing problem.
Step-by-step: when surgery may be the right option
1. Notice whether the symptoms are ongoing
Surgery usually comes up in the conversation when symptoms aren’t occasional or minor. If you’ve had constant nasal blockage, trouble breathing through one side of the nose, mouth breathing, snoring, recurring sinus pressure, or frequent nosebleeds, those patterns may point to a structural issue instead of short-term congestion.
2. Think about how much it’s affecting daily life
A deviated septum doesn’t always need treatment. The bigger question is whether it’s making it harder to sleep well, exercise comfortably, breathe clearly, or get through the day without ongoing frustration. When symptoms start affecting comfort and quality of life, it makes sense to look more closely at the cause.
3. Review what you’ve already tried
Some patients improve with non-surgical treatment such as saline rinses, allergy care, nasal sprays, or other medical treatment. If those options haven’t provided enough relief, that may be a sign that the problem is more structural than inflammatory.
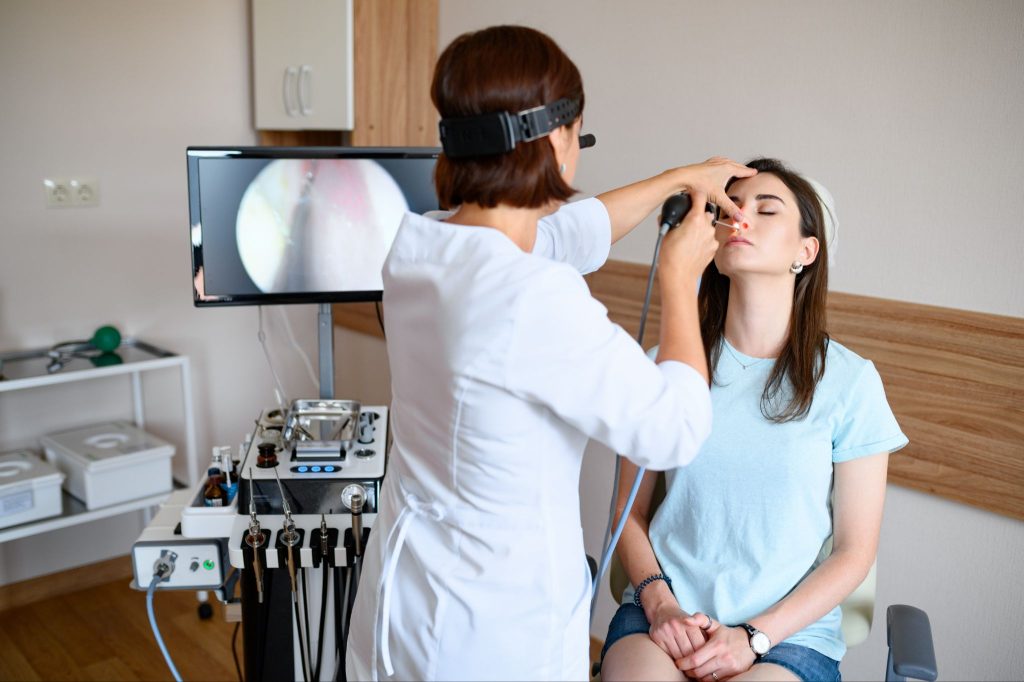
4. Get a full ENT evaluation
An exam helps determine whether the septum is actually causing the blockage. Allergies, enlarged turbinates, inflammation, and other nasal issues cause similar symptoms.
5. Compare your symptoms with the anatomy
Even if the septum is deviated, that doesn’t always mean surgery is necessary. The key is whether the exam findings match what you’re feeling. If the deviation is significant and lines up with your breathing problems, surgery may be more likely to help.
6. Rule out or address other contributing issues
Some patients have more than one reason for nasal obstruction. If allergies, chronic inflammation, or other structural issues are also part of the picture, those may need treatment too. A good evaluation helps you consider surgery for the right reasons.
7. Decide whether surgery is likely to improve airflow and comfort
If symptoms persist, the exam supports this, and medical treatment hasn’t helped enough, septoplasty may be a reasonable next step. The decision should still be balanced. A deviated septum operation can be helpful, but it also comes with healing time, temporary discomfort, and realistic expectations about recovery.
When septoplasty may or may not make sense
Some patients have long-standing nasal obstruction that doesn’t fully resolve. They may feel more blocked on one side, have trouble breathing at night, or feel congested no matter what they try. In those cases, a deviated septum may be a contributing factor.
Allergies, inflammation, enlarged turbinates, or a combination of issues also cause similar symptoms. That’s why you shouldn’t base surgery on symptoms alone. The procedure tends to make the most sense when a deviated septum is clearly contributing to the blockage and other appropriate treatments haven’t provided enough relief.
Benefits of septoplasty
For the right patient, the biggest benefit is improved airflow. If a crooked septum is blocking the nasal passages, straightening it may help the nose feel more open and functional.
Other potential benefits include:
- Easier breathing through the nose
- Less daily congestion caused by structural blockage
- Better comfort during sleep
- Less mouth breathing at night
- Improved quality of life when symptoms have been ongoing
- A clearer path forward after months or years of frustration
Some patients also feel relieved having an answer. When symptoms have been persistent and treatments haven’t worked, understanding that there’s a structural reason is validating. In those cases, surgery may feel less like a drastic step and more like a practical solution.
Another benefit is that this procedure is typically done inside the nose, so there usually isn’t an external scar. For many patients, that makes the idea of surgery feel more manageable.
Still, it’s important to keep expectations realistic. Surgery may improve airflow, but it won’t solve every nasal problem if other issues are also contributing.
Cons of septoplasty
The biggest drawback is simple: it’s still surgery. Even when it’s a common ENT procedure, it comes with risks, healing time, and temporary discomfort.
Potential downsides may include:
- Swelling and congestion during healing
- Bleeding or drainage in the early recovery period
- Temporary discomfort or pressure
- Time away from exercise and normal routine
- The possibility that some symptoms may still need additional treatment
- The chance that surgery may not fully resolve every cause of nasal obstruction
A deviated septum operation helps the right patient breathe better, but it isn’t a cure-all. If allergies, inflammation, or another structural issue are also part of the problem, surgery may improve some symptoms without solving everything on its own.
Patients also need to be prepared for the short-term tradeoff. The nose may feel more congested before it feels better. That would be frustrating if someone expects instant relief. Knowing what the healing process actually looks like helps patients feel more confident and less caught off guard.
What septoplasty recovery is really like
For many patients, recovery is a major deciding factor. It’s normal to wonder how uncomfortable it will be, how long it will take, and when breathing will actually improve.
The first few days often involve swelling, pressure, congestion, and some drainage. Most people describe it as more uncomfortable than painful. The nose may feel blocked during early healing, which can be frustrating if you were hoping to breathe better right away.
During the first week of recovery, patients usually need to rest, keep their head elevated, avoid strenuous activity, and follow post-op instructions closely. Depending on the type of work they do and how they’re feeling, many people return to lighter routine activities fairly soon. Still, exercise and heavy lifting usually need to wait.
As healing continues, swelling gradually improves. Breathing may feel better in stages rather than all at once. You need to give the nose time to settle and heal properly.
What helps most during this period is preparation. Patients tend to feel more confident when they know to expect temporary congestion, some downtime, and gradual improvement rather than an overnight change. A calm, realistic mindset makes the whole process feel much more manageable.
Common mistakes people make when considering surgery
- Assuming every deviated septum needs surgery
Many people have a deviated septum without needing treatment. Doctors usually consider surgery when symptoms are significant and affect daily life.
- Expecting surgery to fix every kind of congestion
Not all nasal blockage comes from the septum. Allergies, inflammation, and other nasal issues may still need treatment.
- Waiting too long to get ongoing symptoms evaluated
Some patients spend years assuming poor breathing is something they have to live with. An evaluation helps clarify the real cause.
- Underestimating recovery
It’s easy to focus on the long-term benefit and forget the short-term healing process. Knowing what septoplasty recovery involves helps patients plan better.
- Confusing function with appearance
Doctors usually perform septoplasty to improve breathing.
What to keep in mind when weighing the decision
- A deviated septum is common, but surgery isn’t always needed
The key question is whether it’s causing enough blockage or discomfort to affect daily life.
- Symptoms matter as much as anatomy
A septum may appear deviated on an exam without being the main cause of breathing problems.
- Clear diagnosis leads to better decisions
Surgery helps most when the septum is truly contributing to the blockage.
- Realistic expectations matter
Understanding what surgery can and can’t do helps patients feel more prepared.
- Treatment should be patient-specific
The real question is whether septoplasty is likely to help this patient with these symptoms.
- Not every patient is the same
Some patients are strong candidates, while others may do better with a different approach.
Helpful tools and care recommendations
Whether you’re managing deviated septum symptoms before surgery or supporting healing afterward, a few simple tools make things easier.
Helpful options may include:
- Saline spray
- Saline rinse, if recommended
- A humidifier for dry indoor air
- Extra pillows to keep the head elevated
- Easy-to-track medication reminders
- Soft foods and good hydration during early healing
- A recovery setup that makes resting more comfortable
If symptoms keep coming back or breathing through the nose never feels normal, it’s worth finding out whether the issue is structural, inflammatory, or a combination of both.
FAQ
Is a septoplasty a major surgery?
It’s usually considered a functional nasal surgery rather than a major surgery in the traditional sense. Still, patients should take it seriously. It involves healing time, follow-up care, and a recovery period that patients should carefully prepare for.
Is septoplasty very painful?
Most patients describe more pressure, stuffiness, and discomfort than severe pain. The early days are still frustrating, especially because the nose may feel blocked before it starts feeling better. Everyone’s experience is a little different.
Will my nose look different after?
In most cases, no. Doctors generally operate to improve breathing. If you also want cosmetic changes, your surgeon may recommend a different procedure or a combined surgical plan.
What is the recovery time?
Septoplasty recovery varies from patient to patient, but the first week is usually the most noticeable part of healing. Swelling and congestion improve gradually, and breathing often improves in stages rather than all at once.

Finding the right next step with Peak ENT
If you’re dealing with ongoing nasal blockage, poor sleep, or trouble breathing through your nose, it may be worth discussing. The right deviated septum operation improves airflow and comfort, but it isn’t the best fit for every patient.A careful evaluation helps determine what’s causing your symptoms and whether septoplasty makes sense. If you’re ready for answers, contact Peak ENT to schedule an appointment.
